|
5/6/2023 0 Comments Als emg findings Motor units have a recruitment frequency of 6–10 Hz and are recognisable by the constancy of the waveform of each discharge (fig 2). 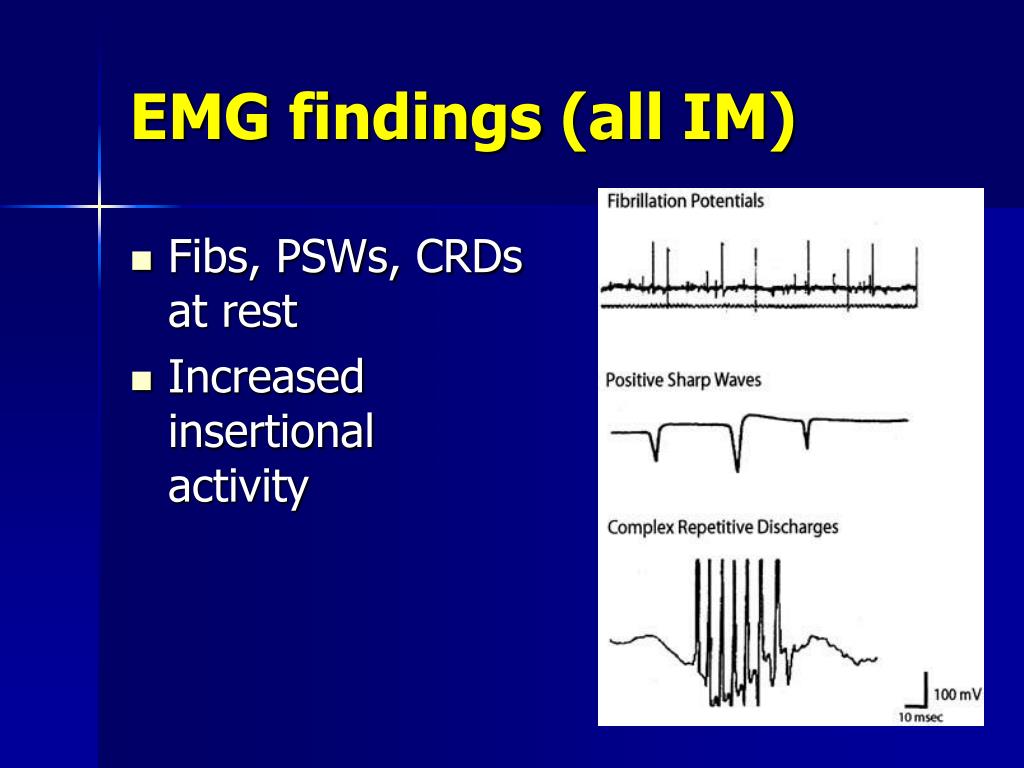
Patients requested to activate minimally a muscle are usually able to recruit a single or a few motor units. EMG is useful in distinguishing myokymia from fasciculation, neuromyotonia and myoclonus. It occurs in a wide variety of conditions, notably with brain stem neoplasms or demyelination and subclinically in episodic ataxia type I. This is the regular or irregular discharge of groups of motor units producing the clinical appearance of flickering in the muscles. Neuromyotonia occurs in autoimmune anti-voltage gated potassium nerve axon channelopathy and Morvan’s syndrome. Neuromyotonia arises from hyperexcitability of single peripheral motor axons either before or after they branch within the muscle, and is characterised by doublet, triplet, or short bursts of high frequency discharge (fig 1B) of motor unit, partial motor unit, or single fibre potentials which produce a “ping” sound from the EMG machine. They occur in muscle fibre membrane channelopathies, including dystrophia myotonica, congenital myotonias, proximal myotonic dystrophy, and hypokalaemic periodic paralysis. Discharges are provoked by needle movement, tapping the muscle and after a short voluntary contraction, and vary in frequency and amplitude producing the characteristic “dive bomber” sound. MyotoniaĬlinical myotonia is accompanied by myotonic discharges on EMG (fig 1D) once heard, never forgotten. The significance of fasciculations is judged by the company they keep in the muscle benign fasciculations are not accompanied by denervation changes but malign fasciculations usually are. Fasciculations occur in motor neurone diseases, other neurogenic diseases such as radiculopathy and neuropathy, thyroid disease, and peripheral nerve hyperexcitability syndromes, and may be benign. 
It has been shown, for example, that there may be more than one generator of a single fasciculation as evidenced by subcomponents of the potential occurring in a different order on different discharges. Fasciculations probably arise within the fine terminal arborisation of a single motor axon within the muscle. Fasciculations are not under voluntary control, a useful point in distinguishing them from motor units discharging due to poor relaxation. Fasciculations near the surface of a muscle may be visible at the skin those deep within the muscle and detected by an EMG needle are not. Fasciculations are isolated discharges that recur at irregular intervals, usually in the order of several seconds. They are larger and more complex than fibrillation potentials. Fasciculationįasciculations arise from the discharge of part or the whole of a single motor unit (fig 1C). They occur predominantly in neurogenic disease. The minimal jitter between potentials suggests that they arise by ephaptic transmission between adjacent fibres. Fibrillations are not found exclusively in neurogenic disease, however they also occur in inflammatory and dystrophic muscle disease.Ĭomplex repetitive discharges begin and end abruptly, may persist for several minutes (or until the electromyographer gets bored), have a constant frequency between 1–100 Hz, and consist of a stereotyped group of single fibre potentials. Any nerve lesion, complete or partial, from the spinal motor neurone to the intramuscular nerve branches can give rise to fibrillation. Fibrillation may persist for many months after a nerve lesion. They arise when the needle tip damages a fibre and spontaneous action potentials propagate up to the needle tip and then are extinguished. Positive sharp waves have the same origin as fibrillation and have the same significance. Fibrillation is not visible through the skin and is an electrical sign not a clinical sign. 
This is detected by the EMG needle as a single fibre discharge or fibrillation (fig 1A). The effect is to make the fibre supersensitive with the result that it discharges spontaneously. Acutely denervated muscle fibres have acetylcholine receptors over the whole of the muscle fibre membrane rather than these being limited to the neuromuscular junction. Muscle fibres themselves remain viable but after a period of 7–10 days become supersensitive and fibrillations will be detectable. SPONTANEOUS ACTIVITY Fibrillation, positive waves, and complex repetitive dischargesĪfter an acute nerve transection, nerve fibres degenerate from the site of the lesion distally. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
